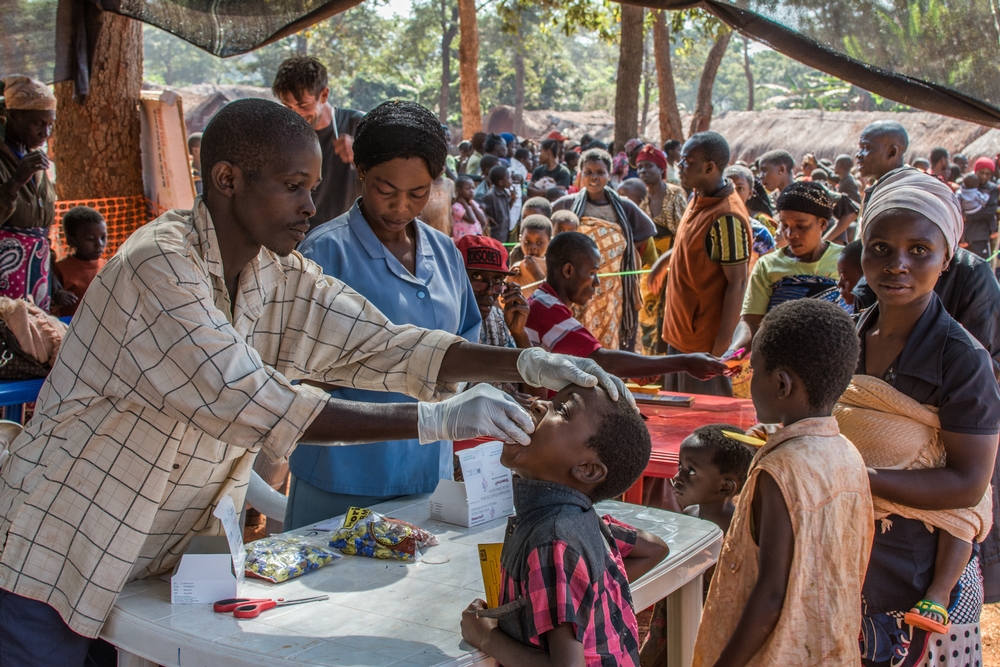
People’s Health Assembly
4-8 December 2000 in Bangladesh
Introduction
In 1978, at the Alma-Ata Conference, ministers from 134 members countries in association with WHO and UNICEF declared “Health for All by the Year 2000” selecting Primary Health Care as the best tool to achieve it.
Unfortunately, that dream never came true. The health status of Third world populations has not improved. In many cases it has deteriorated further. Currently we are facing a global health crisis, characterized by growing inequalities within and between countries. New threats to health are continually emerging. This is compounded by negative forces of globalisation which prevent the equitable distribution of resources with regard to the health of people and especially that of the poor.
Within the health sector, failure to implement the principles of primary health care, as originally conceived in Alma-Ata, has significantly aggravated the global health crisis. Governments and the international bodies are fully responsible for this failure.
It has now become essential to build up a concerted international effort to put the goals of Health for All to its rightful place on the development agenda. Genuine, people-centred initiatives must therefore be strengthened in order to increase pressure on decision-makers, governments and the private sector to ensure that the vision of Alma-Ata becomes a reality.
Several international organizations and civil society movements, NGOs and women’s groups decided to work together towards this objective. This group together with others committed to the principles of primary health care and people’s perspectives organised the “People’s Health Assembly” which took place from 4-8 December 2000 in Bangladesh, at Savar, on the campus of the Gonoshasthaya Kendra or GK (People’s Health Centre).
1453 participants from 92 countries came to the Assembly which was the culmination of eighteen months of preparatory action around the globe. The preparatory process elicited unprecedented enthusiasm and participation of a broad cross section of people who have been involved in thousands of village meetings, district level workshops and national gatherings.
The Plenary Sessions at the Assembly covered five main themes: Health, Life and Well-Being; Inequality, Poverty and Health; Health Care and Health Services; Environment and Survival; and The Ways Forward. People from all over the world presented testimonies of deprivation and service failure as well as those of successful people’s initiatives and organisation. Over a hundred concurrent sessions made it possible for participants to share and discuss in greater detail different aspects of the major themes and give voice to their specific experiences and concerns. The five days event gave participants the space to express themselves in their own idiom. They put forward the failures of their respective governments and international organisations and decided to fight together so that health and equitable development become top priorities in the policy makers agendas at the local, national and international levels.
Having reviewed their problems and difficulties and shared their experiences, they have formulated and finally endorsed the People’s Charter for Health. The Charter from now on will be the common tool of a worldwide citizen’s movement committed to make the Alma-Ata dream a reality. We encourage and invite everyone who shares our concerns and aims to join us by endorsing the Charter.
People’s Charter for Health
Preamble
Health is a social, economic and political issue and above all a fundamental human right. Inequality, poverty, exploitation, violence and injustice are at the root of ill-health and the deaths of poor and marginalised people. Health for all means that powerful interests have to be challenged, that globalisation has to be opposed, and that political and economic priorities have to be drastically changed.
This Charter builds on perspectives of people whose voices have rarely been heard before, if at all. It encourages people to develop their own solutions and to hold accountable local authorities, national governments, international organisations and corporations.
Vision
Equity, ecologically-sustainable development and peace are at the heart of our vision of a better world – a world in which a healthy life for all is a reality; a world that respects, appreciates and celebrates all life and diversity; a world that enables the flowering of people’s talents and abilities to enrich each other; a world in which people’s voices guide the decisions that shape our lives.
There are more than enough resources to achieve this vision.
The HEALTH Crisis
“Illness and death every day anger us. Not because there are people who get sick or because there are people who die. We are angry because many illnesses and deaths have their roots in the economic and social policies that are imposed on us.”
(A voice from Central America)
In recent decades, economic changes world-wide have profoundly affected people’s health and their access to health care and other social services.
Despite unprecedented levels of wealth in the world, poverty and hunger are increasing. The gap between rich and poor nations has widened, as have inequalities within countries, between social classes, between men and women and between young and old.
A large proportion of the world’s population still lacks access to food, education, safe drinking water, sanitation, shelter, land and its resources, employment and health care services. Discrimination continues to prevail. It affects both the occurrence of disease and access to health care.
The planet’s natural resources are being depleted at an alarming rate. The resulting degradation of the environment threatens everyone’s health, especially the health of the poor. There has been an upsurge of new conflicts while weapons of mass destruction still pose a grave threat.
The world’s resources are increasingly concentrated in the hands of a few who strive to maximise their private profit. Neoliberal political and economic policies are made by a small group of powerful governments, and by international institutions such as the World Bank, the International Monetary Fund and the World Trade Organisation. These policies, together with the unregulated activities of transnational corporations, have had severe effects on the lives and livelihoods, health and well-being of people in both North and South.
Public services are not fulfilling people’s needs, not least because they have deteriorated as a result of cuts in governments’ social budgets. Health services have become less accessible, more unevenly distributed and more inappropriate.
Privatisation threatens to undermine access to health care still further and to compromise the essential principle of equity. The persistence of preventable ill health, the resurgence of diseases such as tuberculosis and malaria, and the emergence and spread of new diseases such as HIV/AIDS are a stark reminder of our world’s lack of commitment to principles of equity and justice.
Principles of the People’s Charter for Health
The attainment of the highest possible level of health and well-being is a fundamental human right, regardless of a person’s colour, ethnic background, religion, gender, age, abilities, sexual orientation or class.
The principles of universal, comprehensive Primary Health Care (PHC), envisioned in the 1978 Alma Ata Declaration, should be the basis for formulating policies related to health. Now more than ever an equitable, participatory and intersectoral approach to health and health care is needed.
Governments have a fundamental responsibility to ensure universal access to quality health care, education and other social services according to people’s needs, not according to their ability to pay.
The participation of people and people’s organisations is essential to the formulation, implementation and evaluation of all health and social policies and programmes.
Health is primarily determined by the political, economic, social and physical environment and should, along with equity and sustainable development, be a top priority in local, national and international policy-making.
A call for Action
To combat the global health crisis, we need to take action at all levels – individual, community, national, regional and global – and in all sectors. The demands presented below provide a basis for action.
Health As A Human Right
Health is a reflection of a society’s commitment to equity and justice. Health and human rights should prevail over economic and political concerns.
This Charter calls on people of the world to:
Support all attempts to implement the right to health.
Demand that governments and international organisations reformulate, implement and enforce policies and practices which respect the right to health.
Build broad-based popular movements to pressure governments to incorporate health and human rights into national constitutions and legislation.
Fight the exploitation of people’s health needs for purposes of profit.
Tackling the broader determinants of health
Economic challenges
The economy has a profound influence on people’s health. Economic policies that prioritise equity, health and social well-being can improve the health of the people as well as the economy.
Political, financial, agricultural and industrial policies which respond primarily to capitalist needs, imposed by national governments and international organisations, alienate people from their lives and livelihoods. The processes of economic globalisation and liberalisation have increased inequalities between and within nations.
Many countries of the world and especially the most powerful ones are using their resources, including economic sanctions and military interventions, to consolidate and expand their positions, with devastating effects on people’s lives.
This Charter calls on people of the world to:
Demand radical transformation of the World Trade Organisation and the global trading system so that it ceases to violate social, environmental, economic and health rights of people and begins to discriminate positively in favour of countries of the South. In particular, such transformation must include intellectual property regimens such as patents and the Trade Related aspects of Intellectual Property Rights (TRIPS) agreement.
Demand the cancellation of Third World debt.
Demand radical transformation of the World Bank and International Monetary Fund so that these institutions reflect and actively promote the rights and interests of developing countries.
Demand effective regulation to ensure that TNCs do not have negative effects on people’s health, exploit their workforce, degrade the environment or impinge on national sovereignty.
Ensure that governments implement agricultural policies attuned to people’s needs and not to the demands of the market, thereby guaranteeing food security and equitable access to food.
Demand that national governments act to protect public health rights in intellectual property laws.
Demand the control and taxation of speculative international capital flows.
Insist that all economic policies be subject to health, equity, gender and environmental impact assessments and include enforceable regulatory measures to ensure compliance.
Challenge growth-centred economic theories and replace them with alternatives that create humane and sustainable societies. Economic theories should recognise environmental constraints, the fundamental importance of equity and health, and the contribution of unpaid labour, especially the unrecognised work of women.
Social and political challenges
Comprehensive social policies have positive effects on people’s lives and livelihoods. Economic globalisation and privatisation have profoundly disrupted communities, families and cultures. Women are essential to sustaining the social fabric of societies everywhere, yet their basic needs are often ignored or denied, and their rights and persons violated.
Public institutions have been undermined and weakened. Many of their responsibilities have been transferred to the private sector, particularly corporations, or to other national and international institutions, which are rarely accountable to the people. Furthermore, the power of political parties and trade unions has been severely curtailed, while conservative and fundamentalist forces are on the rise. Participatory democracy in political organisations and civic structures should thrive. There is an urgent need to foster and ensure transparency and accountability.
This Charter calls on people of the world to:
Demand and support the development and implementation of comprehensive social policies with full participation of people.
Ensure that all women and all men have equal rights to work, livelihoods, to freedom of expression, to political participation, to exercise religious choice, to education and to freedom from violence.
Pressure governments to introduce and enforce legislation to protect and promote the physical, mental and spiritual health and human rights of marginalised groups.
Demand that education and health are placed at the top of the political agenda. This calls for free and compulsory quality education for all children and adults, particularly girl children and women, and for quality early childhood education and care.
Demand that the activities of public institutions, such as child care services, food distribution systems, and housing provisions, benefit the health of individuals and communities.
Condemn and seek the reversal of any policies, which result in the forced displacement of people from their lands, homes or jobs.
Oppose fundamentalist forces that threaten the rights and liberties of individuals, particularly the lives of women, children and minorities.
Oppose sex tourism and the global traffic of women and children.
Environmental challenges
Water and air pollution, rapid climate change, ozone layer depletion, nuclear energy and waste, toxic chemicals and pesticides, loss of biodiversity, deforestation and soil erosion have far-reaching effects on people’s health. The root causes of this destruction include the unsustainable exploitation of natural resources, the absence of a long-term holistic vision, the spread of individualistic and profit-maximising behaviours, and over-consumption by the rich. This destruction must be confronted and reversed immediately and effectively.
This Charter calls on people of the world to:
Hold transnational and national corporations, public institutions and the military accountable for their destructive and hazardous activities that impact on the environment and people’s health.
Demand that all development projects be evaluated against health and environmental criteria and that caution and restraint be applied whenever technologies or policies pose potential threats to health and the environment (the precautionary principle).
Demand that governments rapidly commit themselves to reductions of greenhouse gases from their own territories far stricter than those set out in the international climate change agreement, without resorting to hazardous or inappropriate technologies and practices.
Oppose the shifting of hazardous industries and toxic and radioactive waste to poorer countries and marginalised communities and encourage solutions that minimise waste production.
Reduce over-consumption and non-sustainable lifestyles – both in the North and the South. Pressure wealthy industrialised countries to reduce their consumption and pollution by 90 per cent.
Demand measures to ensure occupational health and safety, including worker-centred monitoring of working conditions.
Demand measures to prevent accidents and injuries in the workplace, the community and in homes.
Reject patents on life and oppose bio-piracy of traditional and indigenous knowledge and resources.
Develop people-centred, community-based indicators of environmental and social progress, and to press for the development and adoption of regular audits that measure environmental degradation and the health status of the population.
War, violence and conflict
War, violence and conflict devastate communities and destroy human dignity. They have a severe impact on the physical and mental health of their members, especially women and children. Increased arms procurement and an aggressive and corrupt international arms trade undermine social, political and economic stability and the allocation of resources to the social sector.
This Charter calls on people of the world to:
Support campaigns and movements for peace and disarmament.
Support campaigns against aggression, and the research, production, testing and use of weapons of mass destruction and other arms, including all types of landmines.
Support people’s initiatives to achieve a just and lasting peace, especially in countries with experiences of civil war and genocide.
Condemn the use of child soldiers, and the abuse and rape, torture and killing of women and children.
Demand the end of military occupation as one of the most destructive tools to human dignity.
Oppose the militarisation of humanitarian relief interventions.
Demand the radical transformation of the UN Security Council so that it functions democratically.
Demand that the United Nations and individual states end all kinds of sanctions used as an instrument of aggression which can damage the health of civilian populations.
Encourage independent, people-based initiatives to declare neighbourhoods, communities and cities areas of peace and zones free of weapons.
Support actions and campaigns for the prevention and reduction of aggressive and violent behaviour, especially in men, and the fostering of peaceful coexistence.
A PEOPLE-Centered HEALTH SECTOR
This Charter calls for the provision of universal and comprehensive primary health care, irrespective of people’s ability to pay. Health services must be democratic and accountable with sufficient resources to achieve this.
This Charter calls on people of the world to:
Oppose international and national policies that privatise health care and turn it into a commodity.
Demand that governments promote, finance and provide comprehensive Primary Health Care as the most effective way of addressing health problems and organising public health services so as to ensure free and universal access.
Pressure governments to adopt, implement and enforce national health and drug policies.
Demand that governments oppose the privatisation of public health services and ensure effective regulation of the private medical sector, including charitable and NGO medical services.
Demand a radical transformation of the World Health Organization (WHO) so that it responds to health challenges in a manner which benefits the poor, avoids vertical approaches, ensures intersectoral work, involves people’s organisations in the World Health Assembly, and ensures independence from corporate interests.
Promote, support and engage in actions that encourage people’s power and control in decision-making in health at all levels, including patient and consumer rights.
Support, recognise and promote traditional and holistic healing systems and practitioners and their integration into Primary Health Care.
Demand changes in the training of health personnel so that they become more problem-oriented and practice-based, understand better the impact of global issues in their communities, and are encouraged to work with and respect the community and its diversities.
Demystify medical and health technologies (including medicines) and demand that they be subordinated to the health needs of the people.
Demand that research in health, including genetic research and the development of medicines and reproductive technologies, is carried out in a participatory, needs-based manner by accountable institutions. It should be people- and public health-oriented, respecting universal ethical principles.
Support people’s rights to reproductive and sexual self-determination and oppose all coercive measures in population and family planning policies. This support includes the right to the full range of safe and effective methods of fertility regulation.
People’s participation for a healthy world
Strong people’s organisations and movements are fundamental to more democratic, transparent and accountable decision-making processes. It is essential that people’s civil, political, economic, social and cultural rights are ensured. While governments have the primary responsibility for promoting a more equitable approach to health and human rights, a wide range of civil society groups and movements, and the media have an important role to play in ensuring people’s power and control in policy development and in the monitoring of its implementation.
This Charter calls on people of the world to:
Build and strengthen people’s organisations to create a basis for analysis and action.
Promote, support and engage in actions that encourage people’s involvement in decision-making in public services at all levels.
Demand that people’s organisations be represented in local, national and international fora that are relevant to health.
Support local initiatives towards participatory democracy through the establishment of people-centred solidarity networks across the world.
The People’s Health Assembly and the Charter
The idea of a People’s Health Assembly (PHA) has been discussed for more than a decade. In 1998 a number of organisations launched the PHA process and started to plan a large international Assembly meeting, held in Bangladesh at the end of 2000. A range of pre- and post-Assembly activities were initiated including regional workshops, the collection of people’s health-related stories and the drafting of a People’s Charter for Health.
The present Charter builds upon the views of citizens and people’s organisations from around the world, and was first approved and opened for endorsement at the Assembly meeting in Savar, Bangladesh, in December 2000.
The Charter is an expression of our common concerns, our vision of a better and healthier world, and of our calls for radical action. It is a tool for advocacy and a rallying point around which a global health movement can gather and other networks and coalitions can be formed.
Join Us – Endorse the Charter
We call upon all individuals and organisations to join this global movement and invite you to endorse and help implement the People’s Charter for Health.
PHA Secretariat,
e-mail: phasec@pha2000.org,
link to PHA site
Coordinating Committee:
Asian Community Health Action Network (ACHAN)
Consumers International
Dag Hammarskjöld Foundation (DHF)
Gonoshasthaya Kendra (GK)
Health Action International (HAI)
International People Health Council (IPHC)
Third World Network (TWN)